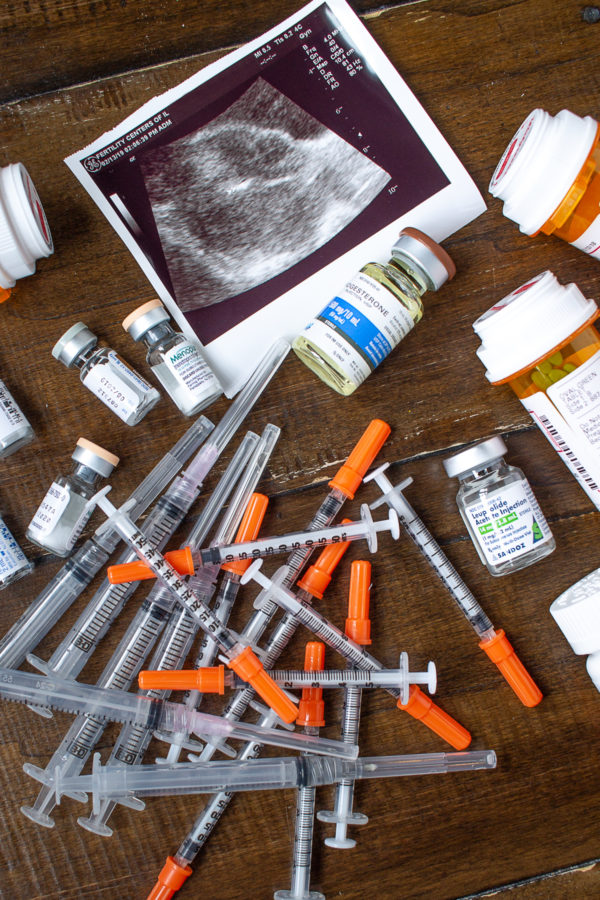
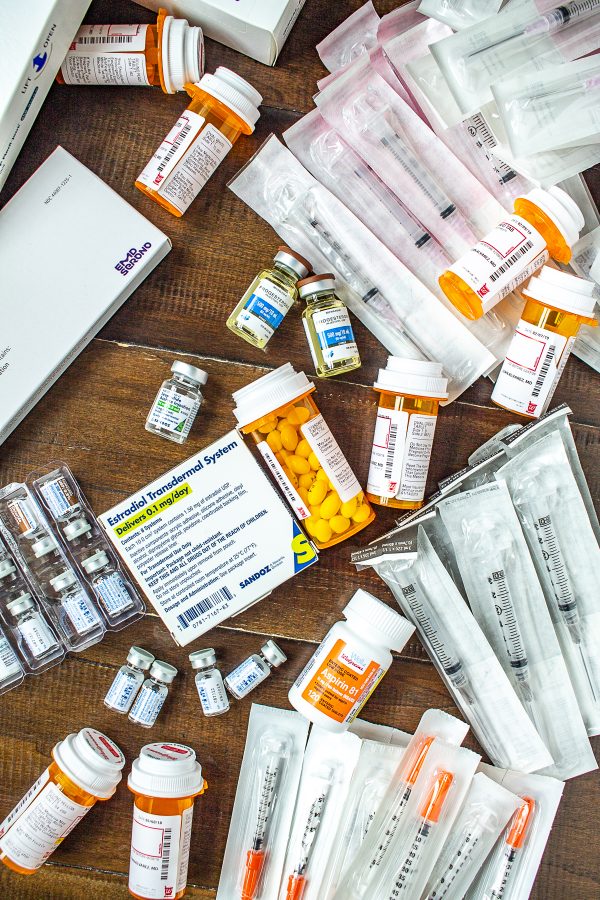
Today I am taking a break from the food and travel content to share the very personal story of my failed IVF cycle. I feel like so few people talk openly about failed IVF cycles, and that it is commonly assumed that if you do IVF that you will have a baby. I'm sharing my story because I want to increase awareness that there are lots of women who have been through this painful struggle.
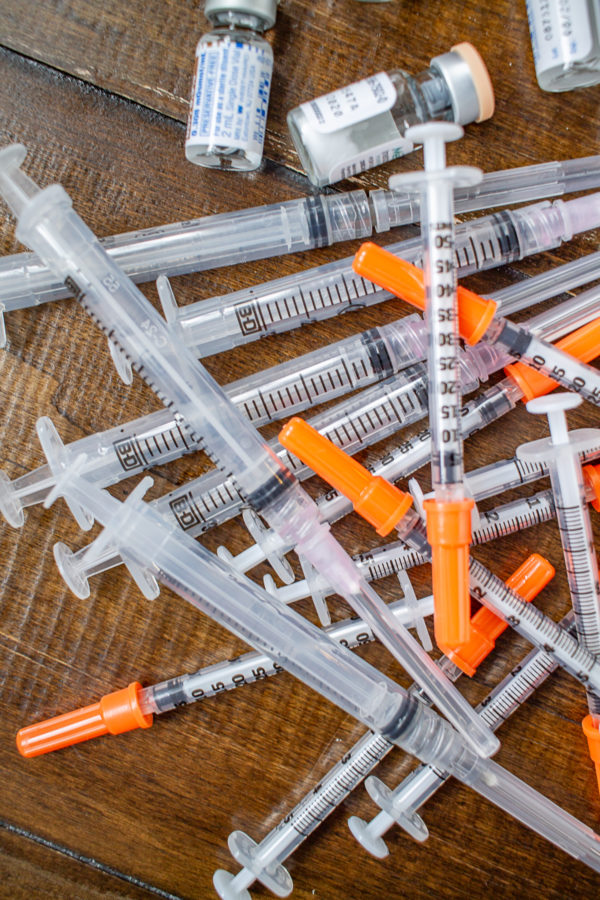
My Failed IVF Cycle:
While I went through one failed IVF cycle, I know that many women have been through this multiple times. I want to acknowledge that there are women who have been through much more than me.
Disclaimer: This is my personal experience, and I am not a doctor.
Summer 2016: The Start of the Story
The story starts three years ago when I was 32. A perfectly healthy 32-year-old with no history of health issues. My mother had three kids in 2 ½ years, so didn't think that I would have fertility problems.
Charles and I always planned on having children, but we weren't in a big rush. We prioritized things like buying a home, traveling, and building my business. After 4 years of marriage, and at the ages of 32 and 36, we were ready. Like many couples, we went from not really trying, to trying, to really trying. What looked like romantic getaways to New York and Europe were often calculated attempts to be together on the right days. After over a year of trying and it not working, we started to realize something might be wrong.
The Diagnosis: October 2017 - March 2018
When I went to my doctor she reassured me. She suggested that we probably just weren’t having good luck with timing. When I asked if we could do a test she agreed and we did a basic blood test to check hormone levels that indicate egg quality and quantity. It was immediately clear that something was wrong.
I got referred to a fertility practice, and through a series of tests, I was diagnosed as a Fragile X Carrier with a Diminished Ovarian Reserve. A year ago I had never heard those terms. Today I have read dozens of articles and research studies, I devoured every article I could find.
Being a Fragile X Carrier and having a Diminished Ovarian Reserve are two separate problems that are often linked. Fragile X Carrier means that I am a carrier for a genetic defect called Fragile X Syndrome. In most cases, genetic defects need to be carried by both parents in order for it to effect a child. Not Fragile X. Fragile X can cause a wide range of birth defects, behavioral problems, and mental disabilities, and it can be passed to a child even if only one parent is a carrier.
According to my intense amount of online research, about 20% of women who are Fragile X Carriers also have a Diminished Ovarian Reserve or trouble with ovarian function. My Diminished Ovarian Reserve means that I don’t have as many eggs as I should. Even though I was 33, my hormone levels were on par with those of a woman in her 40s.
What all of this means is that I have fewer eggs. On top of that, half of those eggs will likely have the Fragile X chromosome which can cause Fragile X Syndrome.
As you can see, things quickly got complicated, and it was determined that IVF was our only option. By the time all of these tests were done, 5 months had passed. Charles and I both went through lots of testing, calls with genetic counselors, and meetings with our doctor.
My IVF cycle was different from what my friends have experienced. Because of my diagnosis, I was given more medications which increased the length of my IVF cycle.
Preparing for the Retrieval: July/August 2018
Between the time of the diagnosis and the retrieval, I started some medications to address a minor thyroid issue. I also had a bunch of blood tests and appointments to make sure my hormone levels were in the right place and to check my uterus. I squeezed in a trip to Provence, thinking it might be the last sister trip that I would get to go on for a while.
When I returned from Provence, I started to prepare my body for the retrieval. I started with one shot each night and some hormone patches. (It seems like not everyone does this step). I got my period as normal, and then I started injections to stimulate my ovaries to produce as many eggs as possible. At this point, an entire shelf in my fridge was for storing medicines. For almost two weeks I was giving myself three shots a day in addition to two pills and two vitamins. I was going to the doctor every other day for bloodwork and an ultrasound. These meds made it hard for me to think clearly. My brain was in a fog, and I couldn't write, a problem when that is your livelihood.
The Retrieval: August 27, 2018
Leading up to the retrieval, I was having ultrasounds to see how many follicles were growing, and it seemed like seven eggs were developing. Even though nurses kept telling me that I had seven follicles, not all of the follicles contained eggs. After the retrieval, we had four eggs, three of which were mature, and two of which became embryos. In just over a week, we went from seven to two. The amount of hope tied to each of the embryos, safely frozen and stored, doubled. Our doctor said that given my diagnosis, we couldn’t hope for a better outcome.
Testing and Waiting: September 2018
Because of my Fragile X diagnosis, we needed to test the embryos to make sure that they were chromosomally normal. Luckily they both were. My doctor recommended that we do another round of retrieval because of my age and the fact that apparently, a 34-year-old's eggs are better than a 35-year-old's eggs. We decided to try transferring an embryo first since we thought another retrieval may not be necessary.
Preparing for the Transfer: October 2018 - January 2019
The next step was for me to go on the birth control pill. Ironically it wasn't working like it was supposed to, and this really held up progress. I needed to have my ovulation suppressed for a period of time before we could do the transfer. Again, I am not a doctor, but I am pretty sure that is what was going on. We had originally planned to do the transfer in November, but it kept getting pushed back. Eventually, after going on a double dose of birth control pills, we were ready to start the protocol for the transfer.
The Transfer: February 2019
I had to do an extra round of shots before the shots for the retrieval, and I had to do an extra round of shots before the shots for the transfer too. First I went on Lupron for ten days, a drug created to treat prostate cancer that has an off-label and not FDA approved use as a fertility drug.
Lupron caused constant mild headaches and big mood swings. At one point I was peeing so much that I had to get tested for diabetes. I don't know of anyone else who had to take Lupron, but I think it was because my body was having trouble staying suppressed.
After Lupron came progesterone in oil, which is progesterone in sesame oil. For the week before the transfer and the two weeks after I had progesterone injections. If injecting hormones and fat into your body doesn’t sound fun enough, it gets better. The needle was long and I ended up with painful bruises and rashes. The sesame oil built up over time and got stuck in my muscles which was extremely painful and took weeks to go away.
The transfer is a surreal experience. You watch as your embryo – just a few cells – is put up on a screen. An ultrasound machine shows your uterus and you watch the two meet. If felt like a pap smear. The entire process took about 5 minutes. As quickly as the team of 4 assembled in the room, they were gone again. The first thing that came to my mind was, “There’s no way that worked.” I don’t know why I thought that. Maybe it is because I felt nothing, and after months of painful blood tests, ultrasounds, and injections I expected it to feel like more. They gave me a photo of the embryo being implanted into my uterus before I left.
I was given valium for the transfer and sent home and to stay on bed rest for the next two days. You have to wait two weeks from the time of the transfer to the time you get to go in for a blood pregnancy test. During those two weeks, Google was my best friend and my worst enemy. I noticed every twinge, cramp, and itch - and the absence thereof. I read message boards and compared my symptoms to others. My brain jumped back and forth from being convinced that it worked, to being convinced that it didn’t.
I entered my transfer date into an online due date calculator and found out that if I was pregnant, I would be due on my birthday. It seemed like a good sign. I was hopeful.
About 10 days after the transfer, and at the time I would usually get my period, I started experiencing sharp stabbing cramps. The kind that wake you up in the middle of the night and keep you up for hours. While the progesterone protocol prevented me from getting my period, I became convinced that the cramps weren't a good sign.
The Pregnancy Test: February 25, 2019
After three days of cramps, the blood test confirmed my suspicions. It didn’t work. I wasn't pregnant. I wasn’t surprised. My gut feeling had been that it didn’t work. A failed IVF cycle is something that you can spend months doing and have nothing to show for in the end, except for thousands of dollars of medical bills. Even with excellent insurance, we spent about $8,000 out of pocket. At this point, we have used up all the IVF cycles that insurance will pay for.
What's Next
At this point, I need a break. For the past 15 months, my life has been dictated by doctor’s appointments and medication protocols. I know that social media didn’t make it look like that, but I wasn't ready to share my story yet and it's easy to use Instagram to make your life look picture perfect. Over the course of 15 months, I went to the doctor over 30 times, had dozens of blood tests, and took over a dozen different medications. I had to suffer through having medication injected into my body over 60 times.
Going through IVF is a part-time job. There were weeks when I was at the doctor's office five times. There were entire days spent dealing with health insurance. It's mentally exhausting and so incredibly time-consuming. At one point it took 5 hours and half a dozen phone calls to resolve an insurance claim that was coded incorrectly by my doctor's office. IVF sucks time out of your life in ways you don't expect.
I have been through a lot physically and emotionally. I know we have one more embryo, but knowing that we already used the “best” embryo I am afraid that it won’t work. Waiting also lets me hang on to the hope a little longer.
It has been a long time since I have felt like me. I want to reclaim my life and my body. I want to do things that bring joy into my life, instead of stressing over an IVF cycle. I am not ready to try again, and I want to give myself time and to try again when I am emotionally and physically ready.
I am disappointed, but I am ok. This very long process has been like a bandaid being very slowly pulled off. It's long and painful and you feel somewhat relieved when it is over.
IVF Etiquette
At my friend's suggestion, I am providing a little guide of what not to say and what to say to someone going through IVF.
Infertility isn’t something many people speak about openly. That confused me for a long time. It isn’t something to be ashamed of or embarrassed about. But then I realized, the reason why people stay so quiet about it is that people say some really insensitive things. And because, the more people you tell, the more people you have to tell when it doesn't work.
Things not to say
If someone tells you they are going through IVF, do not brag about how easily you got pregnant. Yes. This happened. Multiple times. Someone once said, "I think my husband just had to look at me for me to get pregnant the second time."
Do not try to problem solve. If someone has told you that they are going through IVF that means that they have already seen multiple doctors and had an entire series of tests done. Telling them to try drinking a special juice or to read a certain book isn't helpful.
It worked for my friend! Saying that it worked for your friend and that she got 12 embryos isn't helpful unless the diagnosis is similar.
Don't react with excitement that your friend is having a baby. IVF can fail, and it doesn't guarantee anything. Instead of getting excited, just wish them the best.
Things to say and do:
Just listen, check in with your friend. Let them vent.
If you really mean it, offer to help with injections. A reliable person who can assist with shots (especially with the injections into the butt which is hard to reach) is a massive help.
Spend time with them. IVF is a lonely and time-consuming process. There were several weeks when I had to do injections in the evenings and then needed to ice the area afterward. You don't really feel like going out on those nights. It was nice to have friends that would come to my house to hang out with me. IVF killed my social life and seeing friends meant a lot to me.
Be understanding of mood swings and other side effects. Lupron made me crazy. There were times where I was on half a dozen medications, each with their own side effects. I wasn't myself.
If you take anything away from this post, I hope that it is the following:
A simple blood test can help you to understand your egg quality and quantity. You might need to specifically ask your doctor for this test. If I had been tested earlier, my infertility may have been easier to treat.
People who have no health issues otherwise can still have fertility problems.
There are so many reasons why people go through IVF. Lots of women go through IVF because their husbands have a low sperm count. These women don't have fertility issues and their outcome and treatment will be very different from someone like me who has serious fertility problems.
IVF doesn't work for everyone. The way that television shows and movies depict IVF is terribly inaccurate and somehow the woman always gets pregnant in the end, even if she experiences a failed IVF cycle. I wish there was an example of a strong woman who tried IVF, experienced it failing, and went on to have a fulfilling life without children.
The question, "So when are you going to have kids?" can be extremely painful, and it's asked often. I was being asked this so often that I often avoided social interactions.
Thank you for reading this post and my website. It is impossible to express the gratitude that I have for my readers. I am so lucky that I am able to work for myself; creating my own work hours made this difficult process so much easier.
If you want to talk, the best way to reach me is to direct message me via Instagram.
July 2020 Update:
We did a second IVF cycle in the summer/fall of 2019 which was successful! Gwendolyn arrived on July 8, 2020 and we feel so lucky. You can read more about my second IVF cycle here - it involved a failed retrieval and successful transfer of the embryo we had left from the first cycle.